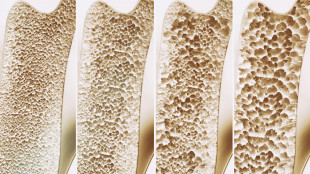
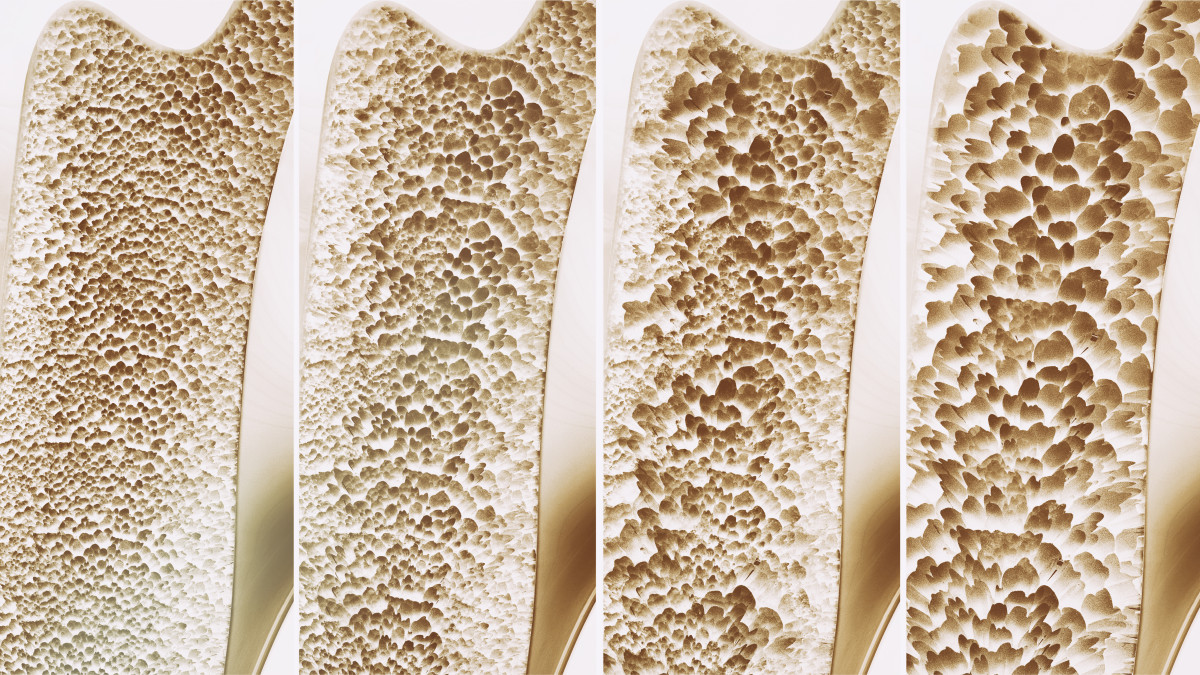
What is osteoporosis?
Osteoporosis is a condition in which bone density reduces to the point where the risk of fractures greatly increases.
Osteoporosis is a serious health issue affecting millions of people, resulting in around 2 million fractures per year. 1 in 2 women and a quarter of men over the age of 50 are likely to experience fractures caused by osteoporosis. These fractures may occur after a fall, but if the bone is badly affected, even carrying out everyday tasks can result in fracture. Osteoporosis has no obvious outward signs or symptoms.
What is osteopenia?
If you have bone loss not significant enough to be osteoporosis, it is considered osteopenia. It can progress into osteoporosis; however, with changes to your diet and exercise along with early treatment, you can minimize the bone loss process.
What causes osteoporosis?
It’s not known for certain what causes osteoporosis, but there are many factors that increase your risk of developing weak and easily broken bones such as:
Risk Factors that Risk factors that
can’t be changed can be changed
· Family History Calcium/Vitamin D deficiency
· Female gender Lack of exercise
· Older age Eating too much protein, phosphorous, sodium,
· Height loss and/or caffeine
· Menopause Lack of fruit and vegetable intake
· Thin/small body type Drinking more than 2 alcoholic drinks per day
Smoking
Medical risk factors
Mobility issues Steroid treatment
Parkinson’s Inflammatory bowel disease (IBD)
Stroke Lupus
Fatigue disorders Rheumatoid Arthritis (RA)
Muscle weakness Organ transplant
Paralysis Sickle Cell disease
Food intake & malabsorption Hormonal imbalances
Celiac disease Prostate/Breast Cancer treatment
Inflammatory bowel disease Diabetes (Types 1 & 2)
Poor diet Thyroid & Parathyroid imbalance
Weight loss surgery Eating disorders
Low male sex hormones
Missed or irregular menstrual cycles
How do I know if I have osteoporosis?
You may not know that you have osteoporosis until a strain, bump, or fall causes a bone to break. A bone mineral density test called a DEXA scan can detect bone loss. This test takes about 15 minutes and can be scheduled for you at your bone health appointment. Lab tests can also be obtained to check appropriate levels of calcium and Vitamin D in your blood which are important for bone health.
Treatment options
Treatment options include supplements, bone building medications, and medications that prevent further breakdown of bone. Taking calcium helps preserve bone quality and Vitamin D helps your body to absorb the calcium. Medications that prevent further breakdown of bone include bisphosphonates, selective estrogen receptor modulators, and RANKL inhibitors and medications that help to build bone include sclerostin inhibitors and PTH analogs. These all aim to reduce your risk of fracture. Ask your provider for more information.
What treatment is available if I fracture my vertebra?
When you sustain a fragility fracture or compression fracture of your vertebra this causes severe pain. This type of fracture is usually associated with osteoporosis. The affected vertebra become wedge shaped and cause shortened height and so-called “dowager’s hump†typical in people who have more advanced osteoporosis.
The technique used at Camelback Spine Care to correct collapsed vertebra is called kyphoplasty.
Kyphoplasty is a minimally invasive procedure that can be done in the office which involves using a small balloon to make space within the collapsed vertebra and then filling it with special material similar to cement, this stabilizes the bone and affords reduction in pain.
.jpg)